HUNTER New England Health has paid out more than $69 million in taxpayer funds for medical mistakes in the past two years, but the local health district will not provide details of the claims, despite having done so in the past.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
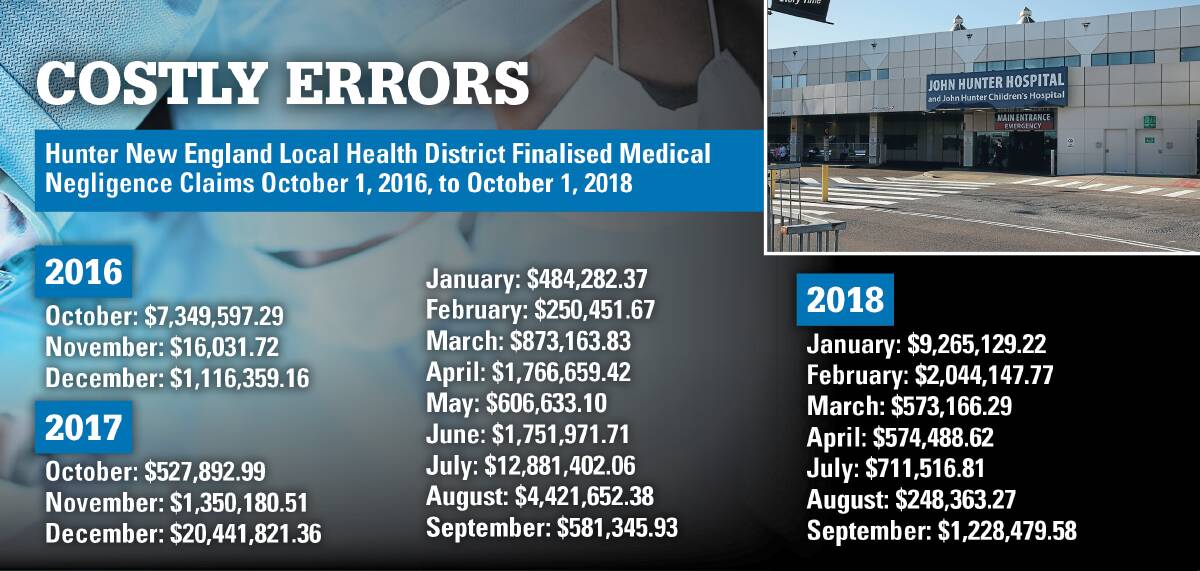
The health district finalised 105 medical negligence claims between October 1, 2016, and October 1, 2018, at an average cost of more than $650,000.
Hunter New England Health (HNEH) paid out more than $20 million in finalised medical negligence claims in December, 2017, alone, documents obtained under the Government Information (Public Access) Act show.
The health district also paid out almost $13 million in July, 2017, and more than $9 million in January, 2018, from Treasury-managed funds.
In its responses to two prior government information requests made by the Newcastle Herald in 2010 and 2015, HNEH provided the individual claim payment amounts and "area of practice" in which the medical errors occurred - such as specialist obstetrics and gynaecology, pathology, or general surgery. Cases ranged from incorrect diagnoses to surgical procedures performed on the wrong body parts.
But HNEH refused to provide this information for the finalised claims between October, 2016, and October, 2018.
An external review by the Information & Privacy Commissioner found HNEH did not meet four of the five grounds relied upon to justify non-disclosure of the information, and recommended the agency make a "new decision".
On review, HNEH would only provide the total net figures in a table showing incurred costs for each month from October, 2016, to September, 2018.
It's decision claimed that providing any further information, with the value of the payments, would make it "reasonably possible" for a third party in "possession of minimal other information" to identify the plaintiff.
It also claimed that sharing the information obtained from "icare Insurance" - also a NSW Government agency - would breach icare's terms and conditions.
Newcastle-based medical negligence lawyer Catherine Henry said this kind of information needed to be readily available to ensure we learned from "avoidable incidents".
She said the figures provided suggested there had been some "catastrophic" claims.
"I'm shocked by these figures - which show that avoidable errors in our region have cost the taxpayer, during a 12 month period from October, 2017, to October, 2018, $46 million," she said.
"Then again we do already know that the John Hunter Hospital is the state's most sued public hospital, with Maitland District Hospital coming in second."
Ms Henry said the global figures provided by HNEH were "not helpful".
"The public has a right to know where the high risk areas are - whether obstetrics, trauma, poor surgical outcomes or unacceptable postoperative outcomes. We don't record data in the way that we need to - to ensure we are learning from avoidable and often tragic incidents.
"We are supposed to have mandated nurse-to-patient ratios in health care.
"The cases we see as medical lawyers are almost universally resulting from systemic issues such as staff shortages. Health professionals in public hospitals are doing long work under severe pressure. Of course mistakes - avoidable errors - will be made."
Lorraine Long, the founder of the Medical Error Action Group, said obstetrics, general surgery and neurology tended to attract the most substantial medical negligence claims.
"All that money could have gone to the hospitals - more nurses, better equipment," she said.
"To get a payout of $700,000, it has to be pretty serious. It is the principle.
"The only way a patient, or a bereaved family, can really show that they're dissatisfied is to sue. You can write to the Minister, the Health Care Complaints Commission, and not get anywhere.
"Patients are very rarely believed. It's a real problem.
"The money doesn't come freely."
Miss Long said sometimes people had operations where other organs were damaged in the process, or were given surgery on the wrong limb or body part.
Her comments came ahead of reports that a cancer patient had the wrong section of his bowel removed at Northern Beaches Hospital after a private-contracted laboratory botched his pathology results.
"We always ask people, 'What do you want out of this?' No one ever says money," Miss Long said.
"They want to see that it doesn't happen to someone else, they want to be heard, and they want the injustice to be righted."
Why is everything a secret? This is our money being spent, and we have a right to know where it is going and why.
- Lorraine Long, founder of the Medical Error Action Group
Miss Long said "every cent" spent on medical negligence claims should be provided to taxpayers.
"They should be fully accountable for every cent," she said. "Why is everything a secret? This is our money being spent, and we have a right to know where it is going and why."
HNEH paid out almost $50 million in the three financial years between 2012 and 2015 for medical mistakes, with more than $11 million going towards specialist obstetrics cases.
Michael DiRienzo, HNEH chief executive said, on average, the district provided care for more than two million patient visits each year.
"This care is at an excellent standard in all but a very small number of cases," he said. "Our most recent data shows clinical incidents across the district have in fact decreased since 2014.
"An increase in costs from medical negligence claims in a particular period is not a reflection of an increase in cases as claims can be submitted up to 21 years after the incident and therefore costs vary from year to year.
"For example, of the 105 claims finalised in the 2016-2018 period, only 22 were initiated in that same time frame."
Mr DiRienzo said the amount of the claim also took into account the patient's personal and family situation, such as their age, dependants and role in their family.
"HNEH endeavours to resolve all claims as quickly and sensitively as possible and provide support for families while a claim is being finalised," he said. "Adverse incidents are reviewed to ensure changes are implemented to avoid errors occurring and full and open disclosure occurs with patients and families."

