
ANGELA Finch arrived for her first ultrasound and mammogram not knowing what to expect.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
She had found a 50 cent sized lump in her left breast two weeks earlier, the day before flying overseas.
Her doctor, who agreed the lump was "unusual", sent her for the tests.
"They told me it was going to cost $800 and as I was waiting to go in the girl said to me, 'You're going to turn 40 in three weeks, if you wait it will cost $200'," Ms Finch said.
"I said 'You know what I'm here for, right? What price do you put on your life?'
"I know she was just trying to be polite, but it was a shock."
Ms Finch's decision to proceed that day proved, unfortunately, to be the right one.
Senior Constable Finch, who works in the Crash Investigation Unit, received her diagnosis eight days before Christmas Day 2018 and 10 days before her birthday.
She had an aggressive malignant invasive duct carcinoma, which was thought to be around 20 millimetres and grade two, but was found after her mastectomy to be 32 mm and grade three.
"It was bigger and worse than what we thought it was," she said.
"What if I had taken her advice to save $600 and come back in three weeks?
"What would have happened? It could have spread. It was a bit of a no-brainer for me."
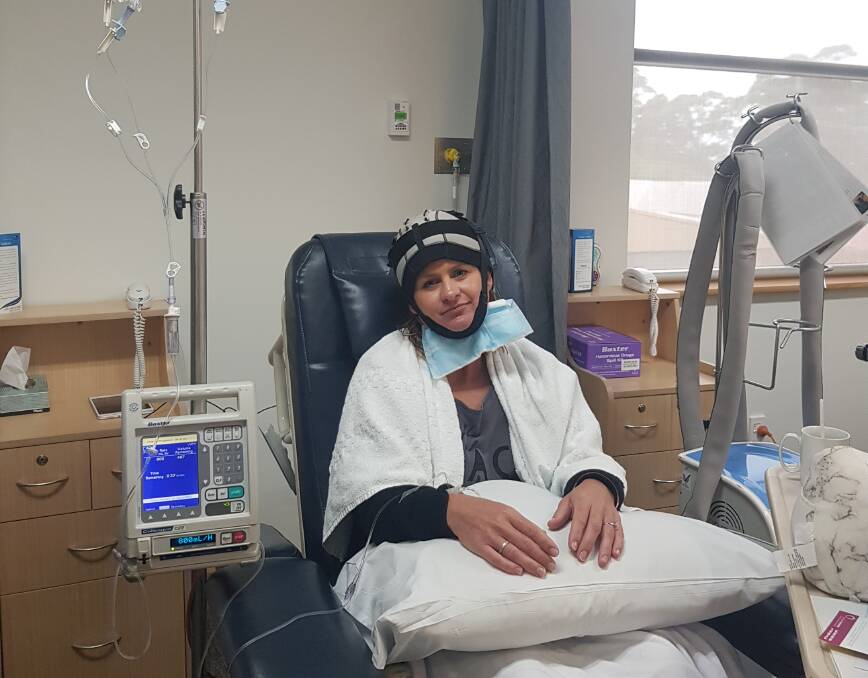
Ms Finch finished her four rounds of chemotherapy in April and is now preparing to have a preventative mastectomy of her right breast on October 24.
"One thing my Mum told me is you've got to learn you're not in control anymore," Ms Finch said.
"You've got all these people telling you what to do, but this was a decision I made for myself.
"I'm taking back control - it does not give me immunity, or mean I won't have cancer anywhere else, but I won't have breast cancer again and that in itself will be a relief.
"When I finish I hopefully can get back to myself again and feel more confident in my own skin, because it really is a confidence basher.
"I have always been really strong, but I felt the whole time like I was going through fight or flight."
Ms Finch said she wanted to share her story to dispel the myth that cancer mostly affects older people and shine a light on the hidden costs and emotional and physical toll of treatment.
She had felt a lump in her breast when she was pregnant with her daughter Stella, now two, but thought it was a blocked milk duct.
She noticed another lump last November, the day before flying to Fiji. While there, her partner Kye Braithwaite proposed and they got engaged.
Ms Finch was booked to return the week after her ultrasound and mammogram for a biopsy, but received a call asking her to come in the following day, a Friday, for the procedure.
Her doctor gave her the diagnosis the following Monday.
"I was feeling numb, thinking 'Are you serious? This does not happen to me,'" she said.
"I felt like I was floating away trying to take it all in."

Ms Finch visited the Breast and Endocrine Centre in Gateshead on December 22 and her surgeon gave her four options: do nothing; radiation followed by a lumpectomy and chemotherapy; a mastectomy followed by chemotherapy; and a mastectomy without any other treatment.
He suggested a mastectomy and chemotherapy.
Ms Finch's family celebrated Christmas Day, Stella's birthday on Boxing Day and her birthday before she returned on December 28 and they discussed her decision to follow his advice.
She booked her mastectomy for January 16.
"It tried to kill me, so I was glad to get rid of it."
She stayed in hospital for five nights before returning home to Hillsborough and starting the slow process of recovery, which included having to be drained twice a week for seromas, or pockets of fluid.
"That's the ugly side of things people don't tell you about," she said.
"It was hard. We tried to shelter Stella a bit from it all. I couldn't lift her and simple chores like hanging the washing out I couldn't do.
"I can't have any trauma on my left side, I can't go in hot spas or saunas, I can't have blood taken from that side anymore because it can cause lymphedema."
Ms Finch saw an oncologist in February, who recommended she start chemotherapy straight away.
She said she did have the option of delaying chemotherapy to try and safeguard her fertility.
"But I decided I'd rather be here for one than dead for two," she said. "It would just take up time."
Ms Finch completed one day of chemotherapy every three weeks for 12 weeks.
She wore a cool cap for an hour before and after each session, which circulated minus four degree water around her head to freeze hair follicles in at attempt to prevent hair loss.
She said it was painful, but credits it with helping to save a third of her hair.
"Four days after the first chemo I was in hospital because of severe nerve pain that I would put in the same class as childbirth," she said.
"Endone did nothing for me and I was on morphine, it was pretty horrific."
She returned to hospital five days later with chest pain. At home she found herself sensitive to noise and light and fatigued, but with insomnia.
"You'd go in for chemotherapy and know two to three days later it was going to hit you.
"I developed a rash all over my body that was like mumps, burning and itchy.
"I had muscle aches, bone aches and ulcers.
"Your mental health suffers as well. I thought I was losing it completely."
Ms Finch said her psychologist hit the nail on the head when she said that despite what Ms Finch encountered at her job, going through cancer treatment was a different kind of traumatic.
She said it was also isolating.
"You just want to shut yourself off from the world," she said.
"Even if you do go out to dinner in a group, some people don't know what to say to you so they say nothing, which is worse.
"When you look in the mirror you don't like what you see anymore so you isolate yourself too.
"After the third round of chemo I did not recognise myself, I was so puffy, my hair was falling out, I had bags under my eyes."
Ms Finch said the testing period was made easier with visits to a gym for cancer patients and the support of her fiancee, family and friends.
"I had really dark days but I had Stella and just had to get on with things as best I could," she said.
"There were days I couldn't look after her and that was upsetting, but she was my main drive - I have to be here for her."
Ms Finch's twin Linda said her sister was a warrior.
"She put in hard work and lived through horror to get to where she is now," Linda said.
"The hardest thing to take out of it was that I could lose her.
"I came into the world with her and it made me realise how precious she was to me."
Linda helped look after Stella, brought goody bags to the hospital, and they spent time together, even if it was watching TV in silence.
"I'm incredibly proud of what she's been through," Linda said.
"It hasn't been easy to see her like this, but she's been incredibly strong."
Ms Finch said she returned to the surgeon after finishing chemotherapy and asked him to remove her right breast, which she had originally asked about at her time of diagnosis.
"I know it's going to be hard," she said of the upcoming surgery.
"I have to have expanders put in [to both breasts] and go back three weeks after surgery to have saline inserted to stretch the skin.
"Then after about three months I'll have the implants put in.
"This surgery alone will cost $8000 because it's seen as a cosmetic procedure, but if I could have my old ones back, if they were fine, then I would not be doing this."
Ms Finch said having cancer had been expensive.
"I went through the private system because if I left it until I went through the public system I would have had a lot harder battle, but there's still so many out of pocket expenses.
"Including physio, medication, all of it, once I finish I would have spent between $15,000 and $16,000.
"Not everybody can afford that. What about people in rural areas?
"This is why a lot of people don't go through reconstruction or preventative mastectomy."
Ms Finch will be on medication for the next 10 years, which aims to ensure any cells not killed by chemotherapy lie dormant.
Side effects again include fatigue, insomnia, muscle and bone aches, as well as dry mouth, hot flushes and night sweats.
She received the results of a genetic test two months ago, which pointed to a hereditary factor.
Her aunt and her late grandmother both had breast cancer.
Ms Finch said that in hindsight, there may have been signs something wasn't quite right.
Returning to work full time, she was frequently doing shift work and on call.
"I always felt tired and was so drained all the time," she said.
"My message is 'Know your body and know when you need to get something checked out'."
Ms Finch refers to cancer as just one of her many life experiences.
"It's always in the back of my mind that it could pop up somewhere else, but if I can say 'I'll never have breast cancer again' then it's a start," she said.
"I take things one day at a time.
"It can break you or make you stronger. I think this did both.
"I feel like I'm a survivor."


