
Tony* moved from Sydney to Newcastle in 1987, devastated by the loss of his partner of eight years to HIV/AIDS. He was also infected with the virus.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
"I just thought I'd be dead in 18 months. It looked to me as if that was the average life span once your were diagnosed," the Newcastle resident, now 80, said.
Tony's partner did not even last that long.
After the couple were diagnosed in June 1985, Tony's partner died of "full blown AIDS" in October the following year. A parasite, that would be harmless to a person with a functioning immune system, entered his partner's brain and caused a series of haemorrhages.
"He died in a deep coma. The doctor said he probably would be able to hear so I sat next to him and kept talking to him until the time he took his last breath," Tony said.
"I believe if he was alive we'd still be together. Now I just live on the memories."

When Tony moved to Newcastle he became one of hundreds of people living with HIV in the Hunter who were treated by staff specialist and clinical director of the Immunology Unit at Royal Newcastle, Dr David Sutherland. The hospital was the only institution in NSW outside of Sydney designated as a centre of care for the testing and treating of HIV/AIDS.
Tony's HIV never progressed to AIDS, and Tony says he has "never had a sick day in his life" due to the virus, an outcome he puts down to Dr Sutherland. The pair met for a consultation every two months for almost three decades, until the immunologist retired in 2014.
"David was on top of everything. He was always monitoring my viral load and T-cells [immune cells], my liver function, kidney function," the octogenarian said.
"It wasn't until 1997 when my T-cells started to drop that he put me on combination therapy and I've just plodded along ever since."
"In the early years we had all received death threats at home. Our offices were broken into many times. People were just wanting to know other people's status."
- Sandy Berenger AM
Dr Sutherland passed away at the age of 76 in Auckland in late October. Tony said the physician was a friend to all his patients.
"He was a lovely man. I miss him very much."
A memorial was held for the Kiwi immunologist at the Newcastle Cruising Yacht Club on Monday, where he was remembered as the man who led the city's response to HIV/AIDS, while influencing national and international policy on the virus as a consultant to the World Health Organisation and delivering training in India, Sri Lanka, Thailand and New Zealand.
The ceremony provided an opportunity to reflect on a moment in Newcastle's history that, Dr Sutherland's long-time colleague Sandy Berenger AM said, "we should never see again".
"David was the person we needed for that season who happened to be in Newcastle. He was able to call us all for action," she said.
The former infection control nurse consultant in the Hunter Area Health Service said the immunologist, who had trained in New Zealand and held research positions in London and Boston, started at the Hunter Immunology Unit in 1983, a matter of months before the city's first known AIDS patients arrived.
"At the time we had no test, no prophylaxis, no medication or therapy. All we had at our disposal was to educate," she said. "David undertook the writing of the layperson's guide to the disease and he wrote the infection control policy and procedure manual all by April 1984, just before our first known patient was cared for at the Royal."

Ms Berenger said Dr Sutherland and his wife Ann had intended to stay in the city for two years. Instead, the pair committed themselves to a "tight-knit" team of health professionals and volunteers who were attempting to support the growing numbers of sufferers of a disease that, at the time, was not only a death sentence but a subject of stigma, paranoia and frenzy.
"During the early years we had all received death threats at home," Ms Berenger said. "Our offices were broken into many times. People were just wanting to know other people's status. But no one got anything. The media caused the community to be fearful of the real facts."
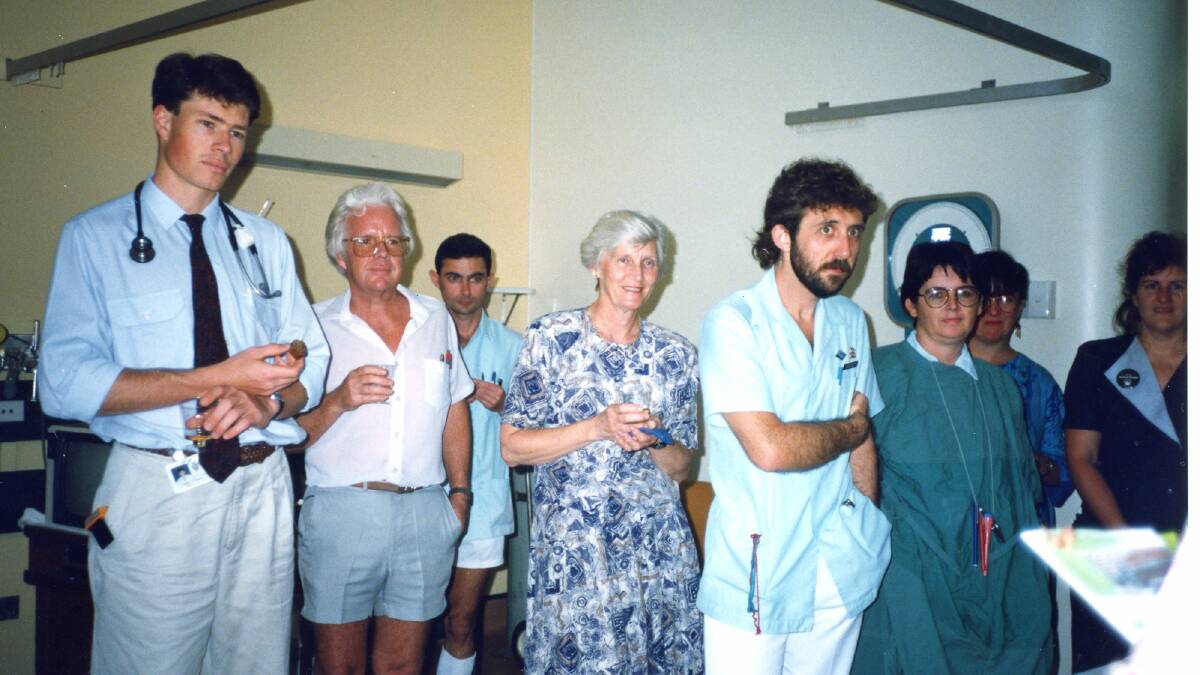
Ms Berenger, Dr Sutherland and his colleague Dr Allan Cripps, who was in charge of testing for the virus and patient confidentiality in the unit, and their team delivered information sessions in gay bars, pubs, brothels, prisons, schools, and workplaces. Ms Berenger said Dr Sutherland became NSW Health's "go-to" person when HIV/AIDS hit the headlines, and he featured in a number of educational videos.
Dr Sutherland in "AIDS: The Facts"
Wayne Baker, who founded a volunteer coalition in Newcastle the "Gay Support Group" to advocate and care for AIDS sufferers, said the lesbian, gay, bisexual and transgender community were "blessed" to have Dr Sutherland at the helm of the city's response.
He said Dr Sutherland's team worked beside the LGBTQ community, after being introduced by social worker Sarah Evans, allowing the health professionals to learn about out how the disease was transmitted and engender enough trust for people to be tested for the virus.
"They got us to organise one [an information session] at Pipers Nightspot," Mr Baker said, "They wanted to know the truth of our lifestyles. People were standing up and talking about the things they did and they didn't do.
"I got a phone call from Sandy [Berenger] the next morning and she said, 'Can you please meet us, none of us know what any of those expressions mean'. I sat in a room with five people with their mouths just dropped open. And they said, 'OK, I think we are right from here', and they were."
People were telling their friends their sons were dying of cancer.
- Wayne Baker
Newcastle's LGBT community raised funds to make the dedicated AIDS unit in the Royal, opened in 1986, as comfortable for patients as possible. Mr Baker said it was then the Hunter AIDS committee at the hospital applied for funding for the Gay Support Group to open a shopfront in Islington, as well as the funding to employ a support worker.
Mr Baker said despite the LGBT community's success in advocating for health resources for AIDS sufferers, it continued to witness the impacts of discrimination on their lives.
Gay Support Group members Geoff Bradley and George Quinn, now 74 and 70, said they were sometimes the only ones to attend the funerals of the men they had volunteered to care for, or the men's families explicitly asked them not to attend.
"People were telling their friends their sons were dying from cancer," Mr Baker said.
He said, however, another "blessing" entered the orbit of AIDS sufferers in Newcastle in the form of a nun: Sister Annie Laurie of the Sisters of St Joseph Lochinvar, who led Dr Sutherland's memorial.
She told attendees she was working in Booragul with single mothers when she read a headline referring to AIDS sufferers as "modern day lepers".
"I thought, 'We have to do something about that.' I went to see David, Sandy and Ann [Bissett, a social worker] and they really checked me out," Sister Laurie said.
She said the team sent her to Kings Cross for two weeks to learn more about the living situations of those who were HIV positive.
"When I came back they realised I was in for the long haul," she said.

Sister Laurie and her fellow sisters were instrumental in securing an old convent in Carrington in 1989 as a house for AIDS sufferers. Sister Laurie was one of four full-time carers at Mackillop House. She said working there was life-changing.
"I fell in love with what really matters and that is to be present for people. David was so much part of that. He became part of our lives when there was a change happening in most of our minds and hearts," she said.
Health professionals who spoke at Dr Sutherland's memorial, said he contributed to many "intellectual journeys" and ensured all staff in his ward, including counsellors and pharmacists, were kept abreast of the latest research on HIV/AIDS.
"David had a calm reassurance which enabled us to care for people without fear," said Pauline Dobson, who was a first-year registered nurse when she began working with him.
He became part of our lives when there was a change happening in most of our minds and hearts.
- Sister Annie Laurie
"I saw him as a dedicated health professional, a fighter for the rights of a group of marginal people and a man who didn't suffer fools readily," said Kerry Todd, who worked as a HIV/AIDS and Hepatitis C surveillance officer.
Dr Sutherland served as director of the clinical immunology unit at the Royal and John Hunter Hospital up until 1993, when he resigned and opened his own rooms in Broadmeadow, where he continued seeing HIV patients, bulk-billed, and others for two decades.

Tony said, thanks to advances in the treatment, his viral load has been undetectable for almost three years, meaning he cab bit pass HIV to others - including his partner of 13 years.
"I'm comfortable with the knowledge that I will die being HIV positive," Tony said, "But I won't die from it."
Ms Berenger said Dr Sutherland's patients were his greatest legacy.
"We need to thank the patients who taught us and changed the model of healthcare delivery in how to provide care," she said.
"We lost so many," she said, "But many are still with us."
*Not his real name
Related stories:

