
Significant concerns have been raised over the NSW regional, rural and remote health system's ability to cope with a potential surge in COVID-19 cases as the state re-opens from its pandemic hibernation.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Submissions and witness testimony to a State parliamentary inquiry that began in September last year paint a picture of an already chronically ill system.
How that system will cope with the added burden of a predicted increase in COVID-19 cases filling beds and ICU wards and requiring transport to and from regional and rural centres to receive expert care has medical professionals and community leaders deeply concerned.
Health Services Union NSW secretary, Gerard Hayes, said our regional and rural health care services were not prepared.
"I'm not saying this to be obtuse, but what we have seen over the past decade has been a system tightening its belt constantly and working to be as lean as possible," Mr Hayes said. "Now as many can work from home, city people are moving to rural locations compounding the pressure already lumped on the health system in these areas as it struggles to cope with a growing population."
A driving force behind the inquiry into health outcomes and access to health and hospital services in rural, regional and remote NSW, 60 Minutes reporter Elizabeth Hayes knows too well the system's flaws.
Ms Hayes' father, Bryan Ryan, died of a stroke at Manning Base Hospital at Taree after he was initially overdosed and then failed to receive his blood thinning medication for eight days.
"In all, it reeks of a system that needs urgent attention," Ms Hayes said. "If anything should be in ICU, it's the rural health system. These are people's lives and whether you're a worker at the coalface or a patient or a family who has had a terrible outcome ... It's devastating."
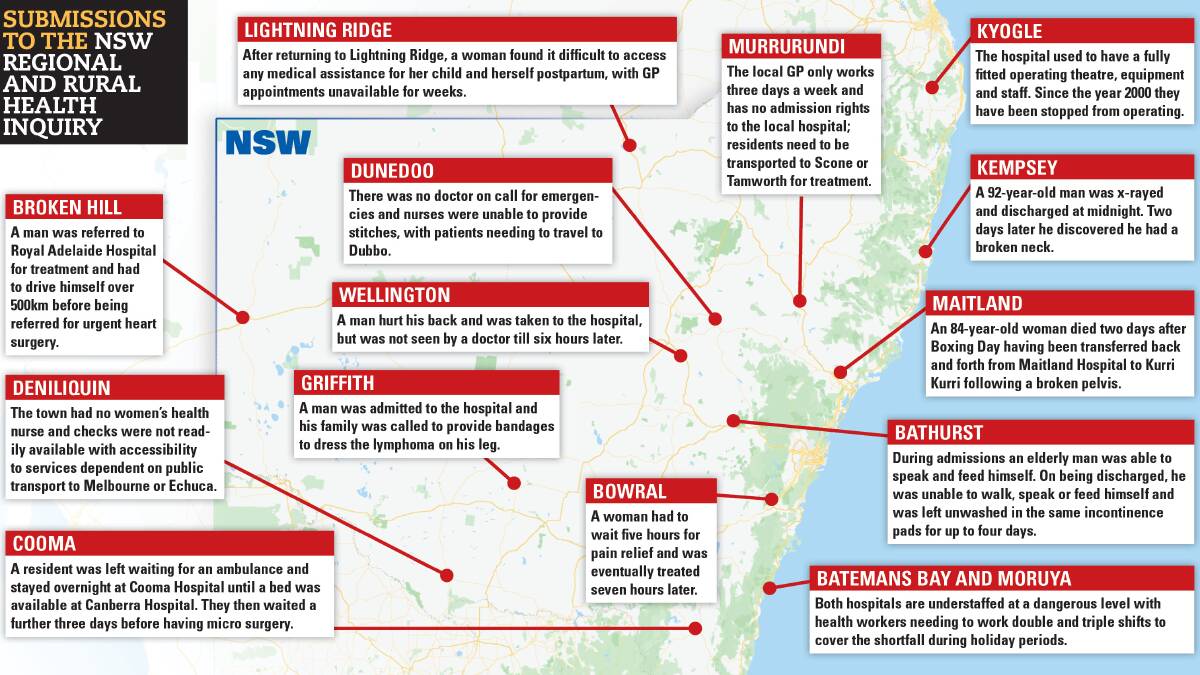
The parliamentary inquiry received more than 700 submissions statewide.
Among them are stories like that of a new mother presenting to Coolah Hospital with suspected appendicitis. She was told she would need to travel to Dubbo Hospital via her own transport because her four-month-old baby couldn't join her in an ambulance.

Twenty-four hours later, she was told she could go home and see what happened or have a CT scan. She opted for the latter.
The CT scan revealed a blocked and twisted bowel with her surgeon remarking "if this had been left [for] another 12 hours, it would have been a very different story".
Another submission tells of an 80-year-old woman who passed away at Cessnock Hospital from a heart condition because there weren't any beds free at Maitland Hospital or John Hunter Hospital.
She had presented to the hospital on three separate occasions with the same condition and had been transferred to the other hospitals which had cardiac equipment.
Earlier this month, the State Government released its roadmap out of COVID-19 lockdowns.
The roadmap, based on modelling by the Doherty Institute, suggested NSW could begin to ease restrictions once 70 per cent of the adult population was fully vaccinated against the virus.
The Doherty Institute has since conducted a "sensitive analysis" of its modelling which was presented to the National Cabinet last week.
The analysis suggests it would be "prudent" to maintain restrictions in areas of concern where there are thousands of cases per day until Australia reaches 80 per cent of the adult population double jabbed.
In a statement, the Institute said, "these findings confirm our earlier strategic advice that even high levels of vaccination will not be sufficient to stop COVID-19 in its tracks".

That could mean an increase in COVID-19 cases across the state as it opens up and an upswing in hospitalisation, patients in ICU and deaths.
"It's every rural and regional health officials nightmare, I would think, and it should be," Ms Hayes said.
"It is obvious hospital healthcare services in rural regions are under-resourced ... They can't cope with what's happening day to day.
"They know that they are barely getting through with what they have for you or me walking in with a regular event without throwing in a virus that knows no boundaries."
At the coalface, there is fatigue. Health advocates and professionals described a dedicated workforce of nurses, doctors, paramedics and other professionals, but also a workforce weary off the back of two years of fire, flood, a mouse plague and the pandemic.
"We are at a critical point where we will start seeing doctors burn out next year from working extra hours, there will be those charging a greater gap because business costs have gone up and there will be no general practitioners for new patients in the area," Dr Debra King, North Coast representative on the Royal Australian College of General Practitioners NSW board said.
"This all results in a rise in chronic illness because people won't be attending their doctor regularly and they will attend hospital emergency departments instead. General practitioners are getting burnt out with the increased workload. Our workforce doesn't go up, we just work longer hours."
It is a message repeated by Scott Beaton, vice-president of the Australian Paramedics Association and paramedic based in Gilgandra.
"We've seen an increase in workload obviously in Dubbo and those areas where there are high amounts of COVID positive patients," he said.
"So we not only have our normal workload to deal with, but then we're topped up with more problems from the extra patients requiring hospitalisation or transport to the hospital for COVID issues.
"Obviously in regional NSW we have a limited amount of health resources. Any extra stress or strain on regional and rural health is going to cause a serious issue."

